MyHumana is a secure online portal with tools to manage your plan. Sign in or activate your account to get safe, immediate access to your plan information. Then, take your Humana essentials with you wherever you go with the MyHumana mobile app.

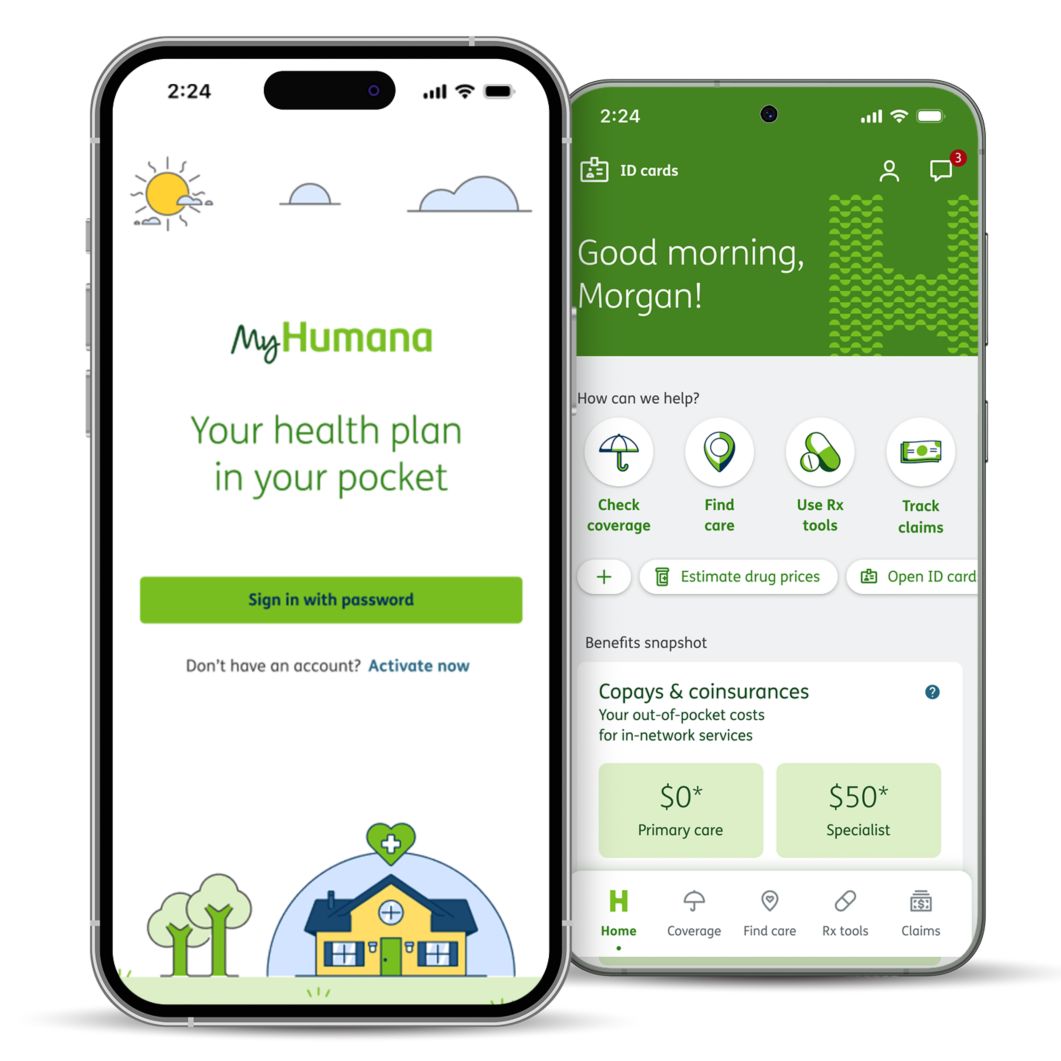
MyHumana on the go
Humana is here whenever you need us. Get the most out of your plan with a MyHumana account, and take your Humana essentials wherever you go with the MyHumana mobile app. Depending on your plan, you can use the app to:
- Explore coverage and benefit details the moment you need them
- Get Humana member ID cards and add them to your phone’s wallet
- Estimate drug prices and check for alternatives before you even leave the doctor’s office
- Pay your premiums on the go
- Find care close to you and get directions on your phone’s map app
Download the MyHumana App for iOS and Android
Activate your MyHumana account
If you need to activate your account, follow these steps:
- Go to the
Start your online Humana profile activation opens in new window page. - Choose “I’m a Member” and select the “Start activation now” button.
- Select your member type and enter your ID number, date of birth and ZIP code.
- Enable 2-factor authentication so you can verify your identity when signing in.
- Set up your profile.
Access your MyHumana account
If you already have an account,
More online resources
View your plan documents online
Enter your Humana Member ID, date of birth and ZIP code to access your electronic Medicare plan documents.
Get help and support
Need a hand? Get help signing in to your account, using your plan and much more.

