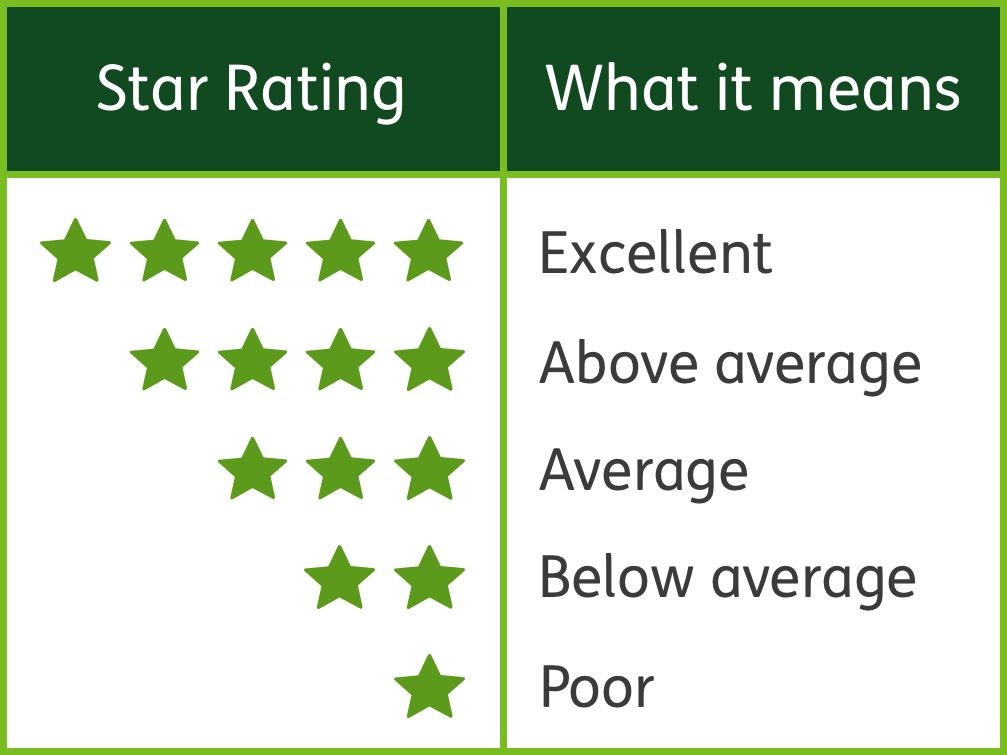
Here are just a few things Star ratings can show you.
How current members rated the plan
Did the Medicare plan provider make it easy for them to get the care they needed, when they needed it? Was customer service helpful and courteous on the phone?
How a plan performed based on industry standards
Were members able to take advantage of preventive care their plans provide, like flu shots or blood pressure screenings? Did the plan provide tools to help them manage chronic health issues like diabetes or rheumatoid arthritis?
How the plans you’re interested in compare to each other
Once you’ve narrowed down your plan choices, comparing their Star ratings may help you make a final decision.
Why are Medicare Star ratings important?
The federal Medicare program provides financial rewards to insurers for highly rated plans. Insurers may use those rewards to reduce member premiums, copays, deductibles or to beef up a plan’s added benefits. So a 4- or 5-Star plan may include extras like dental, vision and hearing coverage. And that additional coverage may help lower your out-of-pocket healthcare costs.
Start with what matters most to you
In 2024, the typical shopper had 43 Medicare Advantage plans available to them.1 That’s a lot to sort through!
Here are just a few things to consider when choosing your Medicare coverage:
- Is your doctor in the plan’s network?
- Are the drugs you’re taking included in the list of covered drugs?
- Are there preferred cost-sharing pharmacies in your area?
- Is the plan affordable?
Once you’ve answered the big questions and narrowed down your plan choices, you might want to consider the Star rating Medicare has assigned to each plan.