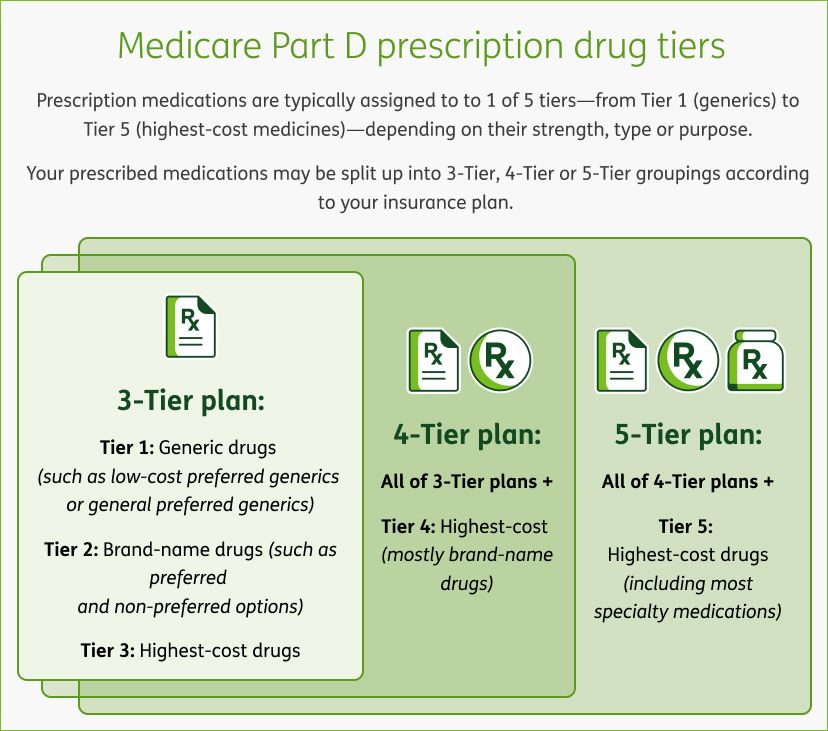
If your specific drug is not on the formulary, there are several actions you can take.
Use a similar drug on the formulary
In most cases, a similar drug to your specific drug should be available. If you or your prescriber believes none of the drugs on your plan’s formulary will work for your condition, you can request an exception.
Request a formulary exception
A formulary exception asks a provider to cover a drug not currently on its drug list. It may also ask a provider to waive a step therapy drug requirement or to waive quantity or dosage limits on a drug. For more information, check out this information on exceptions opens in new window .
File an appeal
If your exception is denied, you can file an appeal to ask the provider to reconsider their decision. Also called a redetermination, the appeal can be filed by you, your representative , your doctor or a non-physician prescriber. Explore these details on Medicare Part D Coverage Redetermination to learn more.
Pay out of pocket
If you’re unable to win the appeal, you must pay 100% of the costs out-of-pocket for all drugs considered “non-formulary.” Paying for these uncovered medications does not count towards your plan deductible or annual out-of-pocket max.